|
Fitness Blog Covering Topics Of Interest Tuesday, December 31 2013
One night, you're in a bad neighborhood. A grungy thug comes out of nowhere and starts chasing you down the block. Suddenly, you are able to run faster and longer than you thought you ever could. And this is because your sympathetic nervous system has taken charge, which stimulates your adrenal glands to work harder. But say you have a work assignment that is due the next day, the baby is crying even though you need to get dinner ready for your guests, your other child is screaming at you, and the TV is on full blast in the other room. Your body still interprets this as being under severe stress. The sympathetic nervous system has a hard time shutting off, the adrenal glands are overworking, and problems occur. Unfortunately, modern life often has overstimulation and a lot of pressures and difficulties that keep the sympathetic nervous system in fight-or-flight mode continually. So where exactly are the adrenal glands? The kidneys are located in the lower back region, right around the second lumbar section of the spine just under your waistline, depending on the person. The adrenal glands are situated right above the kidneys. The body is a whole universe with an extensive communication network. The body's nervous system breaks down into two parts: the central nervous system and the peripheral nervous system. The autonomic nervous system is part of the peripheral nervous system. The autonomic nervous system is responsible for involuntary movements and actions. It controls heartbeats, breathing, digesting, sweating, crying, etc. It is divided into the sympathetic and the parasympathetic nervous systems. The sympathetic nervous system controls the fight-or-flight response. This means how your body responds to emergency and stressful situations. When the sympathetic nervous system is switched on your parasympathetic nervous system is switched off so that your body can cope with the emergencies more efficiently. When the sympathetic nervous system is on your heart rate increases, you sweat, your pupils dilate, and your body shuts down your digestion system so that it can focus on dealing with the emergency. The parasympathetic nervous system kicks in when the sympathetic nervous system switches off. Your heart rate returns to normal, your digestion system starts back up, and body functions return to normal. Although the nervous system's main communicators as neurons, the endocrine system's main communicators are chemical messengers known as hormones. Hormones are carried in the bloodstream to specific areas of the body, including organs and body tissues. Some of the most important endocrine glands include the pineal gland, the hypothalamus, the pituitary gland, the thyroid, the ovaries, and the testes. When the sympathetic nervous system has been in flight-or-fight too long, it affects the hormones of the adrenal system. Too little or too much of the hormones can lead to adrenal fatigue and because of the way this fatigue impacts the body, it can lead to illness. This process of adrenal fatigue does not happen all at once. Instead, it is a gradual breakdown in the body. The Three Phases of Stress In 1956, endocrinologist Dr. Hans Selye developed a key concept in the study of stress and its effects on the body, which he termed, the general adaptation syndrome. In the general adaptation syndrome, the body passes through three phases in the way it copes with stress:
1. Alarm Phase This can cause those raised knotted shoulders, tight upper back and neck, chills along the spine, clammy hands, cold feet, increased heart rate, a tight locked pelvis, and tight leg muscles. A good example of this is in someone who has just had a car accident - a hugely stressful event. Just as their body responds to stress by causing the upper back and legs to tighten, the muscles are jerked quickly, causing injury that can take time to heal. On the other hand, the body does this to stay alive, so that the heart can keep pumping blood even under poor circumstances, and so the person won't feel pain as quickly - that's the beauty of the sympathetic nervous system's response. In the alarm phase, stress is relatively short lived and the return back to homeostasis is with ease. A list of what happens during a fight-or-flight response:
Symptoms: Shortness of breath, palpitations, emotional instability, headache, back pain, decrease in frequency and quantity of urination, insomnia, lack of appetite, dizziness, nausea, eye pain, cold hands and feet, tight neck and upper back muscles. Options on how to treat this stage:
2. Resistance Phase In the resistance phase, constantly reacting to stress leaves the body depleted, leading to a general decrease in overall resistance to illness, inflammation, and pain. Stress is wearing the body out even though the body is still resisting it. There is constant energy being sent by the adrenals and sympathetic nervous system to only the most important organs for a flight-or-fight circumstance. For example, since digestion is a parasympathetic function, undigested food begins to enter the colon, causing gas and bloating, and as the body can't pull the nutrients out of food as efficiently, there are less number of important nutrients to keep the body healthy and pain free. Secretion of the adrenal hormones is initially still high, but slows down as they begin to wear out. The sympathetic nervous system weakness leads to sympathetic deficiency. The parasympathetic nervous system begins to become more dominant as it attempts to compensate. The parasympathetic nervous system will switch on and take over, but not because the sympathetic nervous system has switched off, but because it's so exhausted that the parasympathetic nervous system has to pick up the slack so the body can function. What occurs is a constriction of blood vessels such as capillaries and arteries in the brain, excitement of the digestive system, and adrenal gland deficiency along with a whole host of problems listed below. What happens during the Resistance Phase? What kind of patient has moved from the Alarm Phase to the Resistance Phase?
Symptoms:
Options on how to treat this stage: All the recommendations from Stage 1 will help, but here are a few more for the more severe stage 2. All of these should be checked out with a doctor first as you may be having more severe symptoms stemming from stress (for example, high blood pressure):
Stage 3: Exhaustion Stage Possible Consequences of Exhaustion Phase:
Sources - Bodymind Energetics Towards a Dynamic Model of Health. By Mark Seem, Ph.D. Monday, April 22 2013
Our bodies can obtain vitamin D from diet and make it from sun exposure. Even with these two routes for obtaining vitamin D, however, inadequate vitamin D is common, and deficiencies can be found on all continents, in all ethnic groups, and across all ages—a major concern, given the many ways that vitamin D helps protect our health. () There are a number of factors that increase the risk of having inadequate vitamin D, among them, lifestyle, sunscreen use, geographic location, skin tone, age, and body weight.
The bottom line: Low vitamin D can be found in all ethnic and age groups, around the world, for a host of reasons. Even if you are taking a standard multiple vitamin, the amount of vitamin D in most vitamins (400 IU) is not enough to prevent low blood levels. If you suspect that you are at risk of vitamin D deficiency, you can ask your physician to order a blood test for vitamin D. Tuesday, March 05 2013
Vitamin D Deficiency: A Global ConcernIf you live north of the line connecting San Francisco to Philadelphia and Athens to Beijing, odds are that you don’t get enough vitamin D. The same holds true if you don’t get outside for at least a 15-minute daily walk in the sun. African-Americans and others with dark skin, as well as older individuals, tend to have much lower levels of vitamin D, as do people who are overweight or obese. Worldwide, an estimated 1 billion people have inadequate levels of vitamin D in their blood, and deficiencies can be found in all ethnicities and age groups. (-) Indeed, in industrialized countries, doctors are even seeing the resurgence of rickets, the bone-weakening disease that had been largely eradicated through vitamin D fortification. (-) Why are these widespread vitamin D deficiencies of such great concern? Because research conducted over the past decade suggests that vitamin D plays a much broader disease-fighting role than once thought. Being “D-ficient” may increase the risk of a host of chronic diseases, such as , , , and multiple sclerosis, as well as , such as and even the . Currently, there’s scientific debate about how much vitamin D people need each day. The Institute of Medicine, in a long-awaited report released on November 30, 2010 recommends tripling the daily vitamin D intake for children and adults in the U.S. and Canada, to 600 IU per day. () The report also recognized the safety of vitamin D by increasing the upper limit from 2,000 to 4,000 IU per day, and acknowledged that even at 4,000 IU per day, there was no good evidence of harm. The new guidelines, however, are overly conservative about the recommended intake, and they do not give enough weight to some of the latest science on vitamin D and health. For bone health and chronic disease prevention, many people are likely to need more vitamin D than even these new government guidelines recommend. Vitamin D Sources and FunctionVitamin D is both a nutrient we eat and a hormone our bodies make. Few , so the biggest dietary sources of vitamin D are fortified foods and . Good sources include dairy products and breakfast cereals (both of which are fortified with vitamin D), and fatty fish such as salmon and tuna. For most people, the best way to get enough vitamin D is taking a supplement, but the level in most multivitamins (400 IU) is too low. Encouragingly, some manufacturers have begun adding 800 or 1,000 IU of vitamin D to their standard multivitamin preparations. If the multivitamin you take does not have 1,000 IU of vitamin D, you may want to consider adding a separate vitamin D supplement, especially if you don’t spend much time in the sun. Talk to your healthcare provider. Two forms of vitamin D are used in supplements: vitamin D2 (“ergocalciferol,” or pre-vitamin D) and vitamin D3 (“cholecalciferol”). Vitamin D3 is chemically indistinguishable from the form of vitamin D produced in the body. The body also manufactures vitamin D from cholesterol, through a process triggered by the action of sunlight on skin, hence its nickname, “the sunshine vitamin.” Yet some people do not make enough , among them, people who have a darker skin tone, who are overweight, who are older, and who cover up when they are in the sun. ( Correctly applied sunscreen reduces our ability to absorb vitamin D by more than 90 percent. (8) And not all sunlight is created equal: The sun’s ultraviolet B (UVB) rays—the so-called “tanning” rays, and the rays that trigger the skin to produce vitamin D—are stronger near the equator and weaker at higher latitudes. So in the fall and winter, people who live at higher latitudes (in the northern U.S. and Europe, for example) can’t make much if any vitamin D from the sun. (8) Vitamin D helps ensure that the body absorbs and retains calcium and phosphorus, both critical for building bone. Laboratory studies show that vitamin D can reduce cancer cell growth and plays a critical role in controlling infections. Many of the body’s organs and tissues have receptors for vitamin D, and scientists are still teasing out its other possible functions. New Vitamin D Research: Beyond Building BonesSeveral promising areas of vitamin D research look far beyond vitamin D’s role in building bones. And, as you might expect, the news media release a flurry of reports every time another study links vitamin D to some new ailment. These reports can be confusing, however, because some studies are stronger than others, and any report needs to be interpreted in the light of all other evidence. More answers may come from randomized trials, such as the (VITAL), which will enroll 20,000 healthy men and women to see if taking 2,000 IU of vitamin D or 1,000 mg of fish oil daily lowers the risk of cancer, heart disease, and stroke. Here, we provide an overview of some of the more promising areas of vitamin D research, highlighting the complex role of vitamin D in disease prevention—and the many unanswered questions that remain. Vitamin D and Bone and Muscle StrengthSeveral studies link low vitamin D levels with an increased risk of fractures in older adults, and they suggest that vitamin D supplementation may prevent such fractures—as long as it is taken in a high enough dose. (-) A summary of the evidence comes from a combined analysis of 12 fracture prevention trials that included more than 40,000 elderly people, most of them women. Researchers found that high intakes of vitamin D supplements—of about 800 IU per day—reduced hip and non-spine fractures by 20 percent, while lower intakes (400 IU or less) failed to offer any fracture prevention benefit. () Vitamin D may also help increase muscle strength, which in turn helps to prevent falls, a common problem that leads to substantial disability and death in older people. (-) Once again, vitamin D dose matters: A combined analysis of multiple studies found that taking 700 to 1,000 IU of vitamin D per day lowered the risk of falls by 19 percent, but taking 200 to 600 IU per day did not offer any such protection. () A recent vitamin D trial drew headlines for its unexpected finding that a very high dose of vitamin D increased fracture and fall risk in older women. () The trial’s vitamin D dose—500,000 IU taken in a once-a-year pill—was much higher than previously tested in an annual regimen. After up to 5 years of treatment, women in the vitamin D group had a 15 percent higher fall risk and a 26 percent higher fracture risk than women who received the placebo. It’s possible that giving the vitamin D in one large dose, rather than in several doses spread throughout the year, led to the increased risk. () The study authors note that only one other study—also a high-dose, once-a-year regimen—found vitamin D to increase fracture risk; no other studies have found vitamin D to increase the risk of falls. Furthermore, there’s strong evidence that more moderate doses of vitamin D taken daily or weekly protect against fractures and falls—and are safe. So what is the significance of this study for people who want to take vitamin D supplements? A reasonable conclusion would be to continue taking moderate doses of vitamin D regularly, since these have a strong safety record, but to avoid extremely high single doses. This recent finding does present a challenge to scientists who will work to understand why the extreme single dose appears to have adverse effects. Vitamin D and Heart DiseaseThe heart is basically a large muscle, and like skeletal muscle, it has receptors for vitamin D. () So perhaps it’s no surprise that studies are finding vitamin D deficiency may be linked to heart disease. The Health Professional Follow-Up Study checked the vitamin D blood levels in nearly 50,000 men who were healthy, and then followed them for 10 years. () They found that men who were deficient in vitamin D were twice as likely to have a heart attack as men who had adequate levels of vitamin D. Other studies have found that low vitamin D levels were associated with higher risk of heart failure, sudden cardiac death, stroke, overall cardiovascular disease, and cardiovascular death. (-) How exactly might vitamin D help prevent heart disease? There’s evidence that vitamin D plays a role in controlling blood pressure and preventing artery damage, and this may explain these findings. () Still, more research is needed before we can be confident of these benefits. Vitamin D and CancerNearly 30 years ago, researchers noticed an intriguing relationship between colon cancer deaths and geographic location: People who lived at higher latitudes, such as in the northern U.S., had higher rates of death from colon cancer than people who live closer to the equator. () Many scientific hypotheses about vitamin D and disease stem from studies that have compared solar radiation and disease rates in different countries. These can be a good starting point for other research but don’t provide the most definitive information. The sun’s UVB rays are weaker at higher latitudes, and in turn, people’s vitamin D levels in these high latitude locales tend to be lower. This led to the hypothesis that low vitamin D levels might somehow increase colon cancer risk. ( Since then, dozens of studies suggest an association between low vitamin D levels and increased risks of colon and other cancers. (,) The evidence is strongest for colorectal cancer, with most (but not all) observational studies finding that the lower the vitamin D levels, the higher the risk of these diseases. (-) Vitamin D levels may also predict cancer survival, but evidence for this is still limited. () Yet finding such associations does not necessarily mean that taking vitamin D supplements will lower cancer risk. The trial will look specifically at whether vitamin D supplements lower cancer risk. It will be years, though, before it releases any results. It could also fail to detect a real benefit of vitamin D, for several reasons: If people in the placebo group decide on their own to take vitamin D supplements, that could minimize any differences between the placebo group and the supplement group; the study may not follow participants for a long enough time to show a cancer prevention benefit; or study participants may be starting supplements too late in life to lower their cancer risk. In the meantime, based on the evidence to date, 16 scientists have circulated a “call for action” on vitamin D and cancer prevention: () Given the high rates of vitamin D deficiency in North America, the strong evidence for reduction of osteoporosis and fractures, the potential cancer-fighting benefits of vitamin D, and the low risk of vitamin D supplementation, they recommend widespread vitamin D supplementation of 2000 IU per day. () Vitamin D and Immune Function
Vitamin D and Multiple Sclerosis: Multiple sclerosis (MS) rates are much higher far north (or far south) of the equator than in sunnier climes, and researchers suspect that chronic vitamin D deficiencies may be one reason why. One prospective study to look at this question found that among white men and women, those with the highest vitamin D blood levels had a 62 percent lower risk of developing MS than those with the lowest vitamin D levels. () The study didn’t find this effect among black men and women, most likely because there were fewer black study participants and most of them had low vitamin D levels, making it harder to find any link between vitamin D and MS if one exists. Vitamin D and Type 1 Diabetes: Type 1 diabetes is another disease that varies with geography—a child in Finland is about 400 times more likely to develop it than a child in Venezuela. () Evidence that vitamin D may play a role in preventing type 1 diabetes comes from a 30-year study that followed more than 10,000 Finnish children from birth: Children who regularly received vitamin D supplements during infancy had a nearly 90 percent lower risk of developing type 1 diabetes than those who did not receive supplements. () Other European case-control studies, when analyzed together, also suggest that vitamin D may help protect against type 1 diabetes. () No randomized controlled trials have tested this notion, and it is not clear that they would be possible to conduct. Vitamin D, the Flu, and the Common Cold: The flu virus wreaks the most havoc in the winter, abating in the summer months. This seasonality led a British doctor to hypothesize that a sunlight-related “seasonal stimulus” triggered influenza outbreaks. () More than 20 years after this initial hypothesis, several scientists published a paper suggesting that vitamin D may be the seasonal stimulus. () Among the evidence they cite:
A recent randomized controlled trial in Japanese school children tested whether taking daily vitamin D supplements would prevent seasonal flu. () The trial followed nearly 340 children for four months during the height of the winter flu season. Half of the study participants received pills that contained 1,200 IU of vitamin D; the other half received placebo pills. Researchers found that type A influenza rates in the vitamin D group were about 40 percent lower than in the placebo group; there was no significant difference in type B influenza rates. This was a small but promising study, and more research is needed before we can definitively say that vitamin D protects against the flu. But don’t skip your flu shot, even if vitamin D has some benefit. Vitamin D and Tuberculosis: Before the advent of antibiotics, sunlight and sun lamps were part of the standard treatment for tuberculosis (TB). () More recent research suggests that the “sunshine vitamin” may be linked to TB risk. Several case-control studies, when analyzed together, suggest that people diagnosed with tuberculosis have lower vitamin D levels than healthy people of similar age and other characteristics. () Such studies do not follow individuals over time, so they cannot tell us whether vitamin D deficiency led to the increased TB risk or whether taking vitamin D supplements would prevent TB. There are also genetic differences in the receptor that binds vitamin D, and these differences may influence TB risk. () Again, more research is needed. () Vitamin D and Risk of Premature DeathA promising report in the Archives of Internal Medicine suggests that taking vitamin D supplements may even reduce overall mortality rates: A combined analysis of multiple studies found that taking modest levels of vitamin D supplements was associated with a statistically significant 7 percent reduction in mortality from any cause. () The analysis looked at the findings from 18 randomized controlled trials that enrolled a total of nearly 60,000 study participants; most of the study participants took between 400 and 800 IU of vitamin D per day for an average of five years. Keep in mind that this analysis has several limitations, chief among them the fact that the studies it included were not designed to explore mortality in general, or explore specific causes of death. More research is needed before any broad claims can be made about vitamin D and mortality. () |
 |

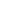

 Vitamin D’s role in regulating the immune system has led scientists to explore two parallel research paths: Does vitamin D deficiency contribute to the development of multiple sclerosis, type 1 diabetes, and other so-called “autoimmune” diseases, where the body’s immune system attacks its own organs and tissues? And could vitamin D supplements help boost our body’s defenses to fight infectious disease, such as tuberculosis and seasonal flu? This is a hot research area and more findings will be emerging.
Vitamin D’s role in regulating the immune system has led scientists to explore two parallel research paths: Does vitamin D deficiency contribute to the development of multiple sclerosis, type 1 diabetes, and other so-called “autoimmune” diseases, where the body’s immune system attacks its own organs and tissues? And could vitamin D supplements help boost our body’s defenses to fight infectious disease, such as tuberculosis and seasonal flu? This is a hot research area and more findings will be emerging.